There are None so Blind…
Written by: Linda Maendel on Thursday, October 19th, 2017
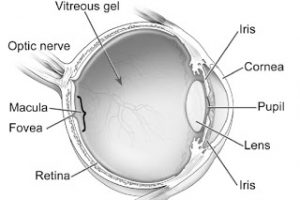
“Your only option is a corneal transplant,” the ophthalmologist stated matter-of-factly.” Although I’d known for years it could one day come to that, I needed time for the reality of having a part of my eye replaced with donor tissue, to sink in.
For years contact lenses provided me with the good vision I lost due to keratoconus, an eye condition in which the normally dome-shaped cornea progressively thins, causing a cone-like bulge to develop. I’m not sure what caused this disorder, but it could have happened when my right eye met a wash line while playing tag at my Hutterite colony as a child. It stung a bit, but not enough for me to complain, or see a doctor. I simply rubbed it a few minutes, stayed in the game and eventually forgot about it. Today, this is hard to fathom, but I obviously got used to distorted vision.
Sometime later, when I noticed blurriness while reading, my parents took me to an optometrist. I came away with glasses, but they never helped my right eye very much. Unaware that other measures might be taken to improve the vision in that eye, I didn’t complain. Nevertheless, I wonder why my optometrist didn’t notice. Not until my late teens and seeing another optometrist, did I learn about the keratoconus. “Your right eye is legally blind. Glasses will never help you,” he informed me. “You’ll have to wear a rigid gas-permeable lens on that eye. It will help straighten the crooked cornea.” I clearly remember the first days with the contact lens: I saw each leaf on the trees separately instead of a blur of green!
Years later the hard lens started irritating my eye, so my optometrist suggested lens piggybacking. Sitting under the hard lens, a soft lens served as protection for the cornea – a perfect solution for decades. However, a few years ago my right eye again started to feel irritated most of the time, to the point where I couldn’t wear contacts at all. The doctor prescribed lubricating eye drops and a variety of lenses, but they were only short term solutions.
Then I was referred to a contact lens specialist in Winnipeg, who had me try different types of lenses as well, all of which continued to irritate my eye. By then I was tired of my sore eye and incompatible lenses. “I believe my eye is trying to tell me that my contact lens days are over.” I told the specialist. “What other options are there?” He referred me to Dr. Rocha, an ophthalmologist in Brandon, MB, thinking corneal collagen cross-linking would be the answer. This technique stiffens the cornea through a combination of exposure to ultraviolet light and eye drops containing vitamin B2. After examining my eyes, Dr. Rocha told me this procedure would be “a waste of your money and my time.” I was down to my last resort, a corneal transplant.
In corneal transplants, the surgeon first decides on either partial or full thickness, based on the condition of the cornea. For my eye, it had to be a full thickness corneal transplant. Next the damaged corneal tissue is removed with an instrument called a trephine, similar to a cookie cutter. The cornea is then replaced with a precisely matched donor corneal graft stitched in place by hair-thin sutures.
Being on a waiting list for over a year, gave me ample time to ponder this option. Questions scrolled through my mind: How successful is this type of surgery? How long does it take for the eye to heal? How often are donor corneas rejected? Over clinic visits and phone calls, my fears were allayed and I was well prepared, when my call came. However, I had one lingering thought: in order for me to receive a donor cornea, someone would have to die. And that person would have chosen to donate his/her organs and tissue.
A corneal transplant is not life-saving surgery like receiving a new heart, kidney or liver, and I can’t imagine how these people feel after surgery. However, it is life-changing; not a day goes by without me thinking about my donor, this person whose final act of love gave me better vision.
When my name was placed on the list, I never expected to have to wait fourteen months for a donor cornea. When I asked Dr. Rocha about the long wait, he explained that there are three reasons: education, systems and processes, and funding.
“More awareness on the part of donors but also health personnel and authorities is needed.” Dr. Rocha elaborated, “Signing the driver’s license as a donor is not enough. Corneal tissue can be harvested within six hours of death, processed within twelve hours and used up to fourteen days later. There is no reason why this should be difficult, other than the lack of knowledge that has prevailed.”
It seems many people are not aware of the need for organs and tissue, or are indifferent. Granted, becoming an organ donor is not a topic that’s readily discussed, but that doesn’t mean it shouldn’t happen, especially since thousands of Canadians are waiting for corneal transplants, not to mention other organs. Had I never been on a wait list, I wouldn’t have thought to inquire about this, and would have remained in the dark about the ongoing issues surrounding corneal transplants. Some of these issues are systems and processes, Dr. Rocha pointed out:
“There are laws for mandatory reporting of deaths depending on the province. It has been estimated that, for example, in Manitoba, ensuring a proper reporting and procurement process in a single hospital, could provide the corneal transplantation needs for the whole province.”
Waiting for a donor cornea has opened my eyes not only to the need for donors, but also the obstacles that hinder doctors from helping patients in need of corneal transplants. It also helped me see things in a new light and made me more receptive of ideas I might not have agreed with before. For example, if someone had told me a few years ago that in Spain, when a person dies it’s legal for doctors to harvest the organs and tissue, I would have been appalled. In Canada, even though someone opted to be a donor, that person’s family can veto this decision. Since the family is already experiencing the trauma of losing a loved one, doctors will not insist, meaning the organs and tissue are lost. Many would likely argue that the Canadian law is right, and Spain’s Presumed Consent Legislation is wrong. For me it comes down to one question: Why bury precious organs and tissue that would greatly benefit other human beings?
The third reason for long wait lists, is a problem that other healthcare areas face as well; government funding:
“A few years ago,” Dr. Rocha informed me, “I was part of a group coordinated by the Canadian Blood Services, tasked with establishing a nation-wide organ and tissue donation. This initiative was prompted by Government. However, after several years of work including meetings and conference calls, when we were ready to proceed, both Federal and Provincial Governments denied further funding for the project.”
Someone in need of a cornea could wait up to two years, because there are not enough donors in Manitoba. Since we lack accreditation across Canada and inter provincial co-operation, surgeons are unable to acquire donor corneas available in other provinces. An example occurred a few years ago when seventy healthy surplus corneas from Quebec were wasted because other provinces only recognize the Eye Bank of America accreditation, disregarding the fact that Quebec’s eye bank has Health Canada accreditation (Moore, 2013). It’s appalling to think that people are going blind when government funding could provide a solution.
We have so much to be thankful for in our country, and some of those blessings were highlighted for me during my corneal transplant: our health care system, hospitals, doctors and their staff. Concerning transplants however, medicine, science, state-of-the-art micro- surgical equipment and skilled surgeons cannot provide anyone with a new cornea or any other organ, without donors and their supportive families.
Prior to my right eye giving me trouble, I never thought about organ and tissue donations long enough to put some action behind the thought. There’s nothing like facing a transplant to lend some perspective: I finally signed up to be a donor! I couldn’t put my name on a wait list, without first declaring my intent to be a donor myself.
Sign Up For Life is the Canadian website where becoming a donor is fairly easy. While it feels strange to click on organs and tissue you’d wish to donate, that only lasts a few minutes. The decision to be a donor can impact a person waiting for an organ or tissue for a lifetime.
Because someone chose to be a donor, I was able to say farewell to keratoconus. Through this journey my eyes have been opened to the issues surrounding corneal transplants as well. The solutions to make our Canadian corneal transplantation system more efficient seem simple enough, if only governments and ophthalmologist shared the same passion and vision for helping people.
“The only thing worse than being blind, is having sight and no vision.” Helen Keller








 If you have any questions, suggestions or feedback or require more information about the hutterites, be sure to contact us
If you have any questions, suggestions or feedback or require more information about the hutterites, be sure to contact us
Showing 2 comments
Paul McKeever said:
On: 15th Apr, 2018 at 00:13
Great story, I’m glad your eyesight has been restored.
Lindamaendel said:
On: 22nd Jun, 2018 at 09:54
Thanks, Paul!